If you regularly spend your nights tossing and turning or feel sluggish all day even after a full night’s sleep, then you could be suffering from narcolepsy or sleep apnea. But what is the difference between sleep apnea and narcolepsy? How do you know which one you have?
Difference between Sleep Apnea and Narcolepsy
Both of these conditions are associated with excessive daytime drowsiness. To put it simply, sleep apnea affects breathing, which is why its most common symptom is snoring. Narcolepsy, on the other hand, affects the sleep cycle itself.
Here’s a deeper look into these two.
Sleep Apnea
Sleep apnea occurs when there is a repeated pause between breathing during sleep. This is characterized by loud snoring during sleep and a feeling of sluggishness and restlessness even after a full night’s sleep.
There are a few types of sleep apnea, which are:
Obstructive Sleep Apnea – This is the most common type, chronic, and potentially life threatening. It causes a higher risk for various health conditions, such as stroke, coronary artery disease, heart failure, hypertension, type 2 diabetes, and more.
Central Sleep Apnea – This takes place when the brain is unable to send the correct signal to the muscle that controls breathing. It’s a disorder that starts and stops throughout the night. This means a person suffering from this condition is unable to inhale efficiently since the airway has collapsed.
Complex Sleep Apnea Syndrome – also referred to as treatment-emergent central sleep apnea, happens to a person with both obstructive and central sleep apnea.
There are a few common symptoms of sleep apnea. Some of them are listed below:
– Snoring
– Gasping for air while asleep
– Insomnia
– Morning headaches
– Hypersomnia (excessive daytime sleepiness)
– Periods where one stops breathing during sleep
Any combinations of these symptoms suggest sleep apnea. It is best to consult with your doctor for a proper diagnosis.
Treatments for Sleep Apnea
Fortunately, sleep apnea is treatable. But since the condition could be a cause of different health conditions, it is important to have it properly diagnosed.
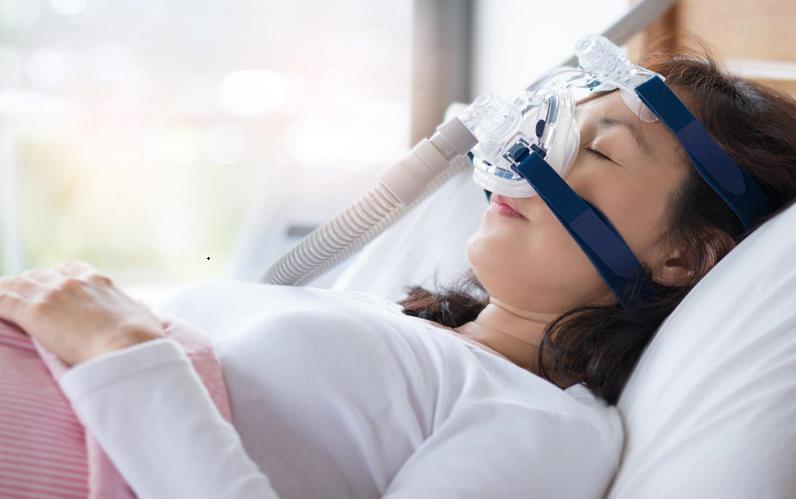
People suffering from obstructive sleep apnea are prescribed with a device called Continuous Positive Airway Pressure Device (CPAP). It’s basically a mask that fits over the nose and/or mouth and pushes air to the airway. It can quickly stop snoring and provide a good night’s sleep.
Another common treatment is in a form of dental appliances. These tools help reposition the lower jaw and tongue and allow proper breathing.
Some more serious conditions may require surgeries like upper airway surgery to remove an obstruction in the air passage (airway tissue).
Other cases may only require a nasal valve, a disposable valve placed over the nostrils for people with nasal valve collapse.
In most cases, sleep apnea is a result of weight gain and lifestyle habits like drinking and smoking. Doctors will always recommend a lifestyle change and require patients to lose weight, as well as avoid alcohol and smoking.
Narcolepsy
Narcolepsy is a rare chronic disorder that disrupts sleep, and not breathing like sleep apnea. It is characterized by sudden sleepiness and daytime drowsiness. Most patients of this condition are at near the age of puberty (15 to 25 years old). Those over 30 years of age are diagnosed with obstructive sleep apnea first, before narcolepsy.
A normal sleep cycle involves two basic stages: the early stage and deeper stage. After around 1 hour and 30 minutes, the body enters the Rapid Eye Movement (REM) stage of sleep. This is when the brain activity increases resulting in intense dreams. People with narcolepsy, on the other hand, go straight into REM stage without going through the first stages. People with this condition often find it extremely difficult to stay awake for long periods of time, causing serious disruptions in their daily routine.
There are two types of narcolepsy, such as:
Type 1 or hypocretin deficiency with cataplexy – abrupt loss of muscle tone (cataplexy), especially during times of strong emotional reactions like anger, laughter, or surprises. This also comes with different levels of disability; some may fall to the ground, while others experience weakness in lower extremities of the body.
Type 2 or hypocretin deficiency without cataplexy – narcolepsy without the episodes of loss of muscle tone (cataplexy).
Below are the common symptoms that are linked to narcolepsy.
– Excessive daytime sleepiness (EDS) – Feeling sluggish, exhausted throughout the day is the most common symptom for narcolepsy. Aside from which, patients of this condition also suffer from memory lapses, decreased alertness, concentration, and focus.
– Cataplexy (loss of muscle tone) – Narcolepsy can lead to multiple physical changes, such as slurred speech, weakness of muscles, etc., which could last for a few minutes.
– Sleep Paralysis – It refers to a temporary loss of ability to move or speak upon waking or while falling asleep.
– Hallucinations – Narcoleptic patients suffer from two types of hallucinations:
-
- hypnagogic hallucination – happens while falling asleep
- hypnopompic hallucination – happens upon waking
– REM sleep changes – disrupts sleep
Treatment for Narcolepsy
Unfortunately, there is no cure for this condition. However, since the symptoms are extremely dangerous, it is important to seek medical help. Sleep doctors can help manage the symptoms and aid patients of this condition to effective lifestyle changes.
Below are some of the recommendations by doctors for patients with narcolepsy:
– Taking brief and frequent naps throughout the day
– Self-care and relaxation techniques before going to bed
– Strict bedtime routine
– Avoid alcohol, caffeine, and smoking before bed
– Exercise at least a couple of hours before bedtime
The most important parts of the management are patient education and a good support system.
If you feel you experience any or combinations of the symptoms for both conditions, it is important to speak to your doctor and get the appropriate help.