An Introduction to Sleep Apnea and TMJ
Sleep apnea and TMJ are actually two very different conditions. Sleep apnea (obstructive sleep apnea or OSA) is a sleep disorder where the breathing pattern is disrupted multiple times a night due to obstruction in the airway. Characterized by snoring, sleep apnea is potentially serious, and disruption to breathing causes inadequate oxygen intake during sleep, leading to poor sleep quality. When left untreated, the condition could develop into numerous health complications, such as digestive problems, high blood pressure, Type 2 diabetes, cardiovascular diseases, sleep deprivation, reflux, increased cortisol levels (fight or flight), and even death.
Temporomandibular Joint Disorder (TMJ disorder, commonly referred to as TMJ), is a problem in the temporomandibular joint – the jaw joint that connects the lower jaw to the skull. These joints are found in each side of your jaw and act like a hinge that allows up and down and side by side movement of the jaw. Stress in these joints caused by wear and tear or other medical conditions results in pain and uncomfortable symptoms such as earache, headaches, neck pain, shoulder pain, and migraines.
Traditionally, sleep apnea and TMJ are treated separately. However, recent studies suggest there is a strong connection between the two. In another study, 43% of patients with TMJ disorder also have sleeping problems such as sleep apnea.
Aside from the obvious proximity between the jaw’s position and the airways, experts explain that when the airway collapses due to sleep apnea (snoring), the automatic and involuntary response of the body is to try to open up the airway by pushing the lower jaw forward. This is a constant motion that happens throughout the night, and due to continued stress, this leads to wear and tear and tension in the jaw joint. This is why the two conditions often go hand in hand.
Subsequently, TMJ disorder is linked to chronic fatigue syndrome (CFS), a complex disorder characterized by extreme fatigue that can last up to six months. This condition cannot be fully explained by any underlying medical condition. The fatigue often gets worse with physical and mental activities, and rest doesn’t seem to help. CFS aggravates sleep apnea affecting the overall health of the individual.
Common symptoms of sleep apnea with TMJ
Here are some of the tell-tale symptoms that could suggest you have sleep apnea and TMJ:
- Tension headaches and migraines, especially in the morning
- Clicking or popping of the jaw
- Jaw pain or jaw soreness, especially when waking in the morning
- Irregular jaw motion
- Earache and stiff feeling around the ear
- Ringing in the ears
- Vertigo
- Back pain, shoulder pain
- Tooth damage caused by wear and tear
- Numbness and tingling feeling of the jaw area
Proper Treatment for Sleep Apnea and TMJ
The problem with both conditions is many people don’t feel the need to address this health concern until they get worse.
For a treatment to be successful, the link between the two must be carefully considered. Fortunately, dentists and doctors alike are trained to recognize the signs. As a matter of fact, by examining the structure of the mouth, a dentist can identify one’s risk of developing sleep apnea.
Wear and tear of the teeth caused by jaw clenching and teeth grinding, a narrow palate, and a scalloped and oversized tongue are common tell-tale signs of sleep apnea.
Some common treatments for TMJ associated with sleep apnea include:
Wearing of mouth guards or oral appliances
Dentists often prescribe custom-fit mouthguards or night guards to patients suffering from sleep apnea. When worn at night, these devices reposition the lower jaw to keep the airway open. Oral appliances like tongue-retaining or mandibular-repositioning appliances effectively stop pauses in breathing by enlarging the upper airway and reducing its potential of collapsing.
Similarly, patients who suffer from jaw clenching and teeth grinding are often prescribed mouthguards by their dentists. This provides a soft cushion between the upper and lower teeth, reducing the tension on the jaw joint during sleep.
For bite splints that are worn at night, however, it is important for the dentist to consider how the appliance repositions the airway. The bite splint must be specially designed so that it doesn’t restrict the airway further and must keep it open.
Also for sleep apnea, the oral appliance must position the jaw where it doesn’t cause any stress to the jaw joint. If the splint causes stress to the TMJ, it will feel uncomfortable and may potentially cause further damage to the joint.
Continuous positive airway pressure (CPAP) machine
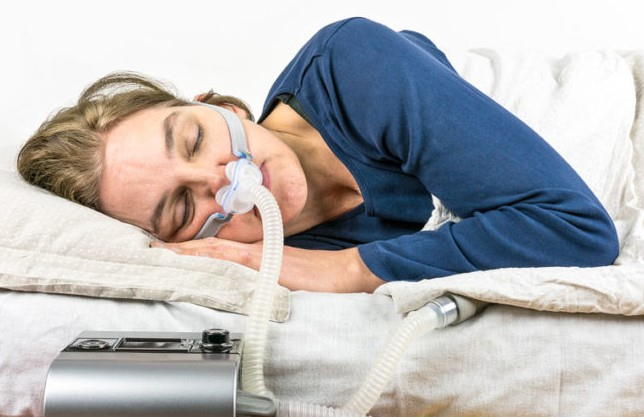
For moderate and severe cases of sleep apnea, doctors prescribe the use of CPAP machines. As a matter of fact, this is the gold standard for OSA treatment. This machine delivers air pressure continuously through a mask that is worn during sleep. The air pressure from the mask is higher than the surrounding air, and just strong enough to keep the airways open. This prevents snoring and sleep apnea.
Though effective and reliable, CPAP machines are cumbersome. Many people give up on this treatment as it is indeed uncomfortable to sleep with a mask on. Not to mention the machine tends to be noisy and distracting at night.
Surgical options
For severe cases that do not respond well to CPAP, surgical interventions like surgical airway correction are considered. This procedure greatly reduces the symptom of sleep apnea by lessening the airway obstruction and improving the strength of the upper airways.
Other surgical procedures include nasal procedures (reduces nasal blockage caused by cartilage, bone, or tissue), Uvulopalatopharyngoplasty (removal of excess tissue from the pharynx and soft palate), Tonsillectomy (for children), Palatal Implants, Hypopharyngeal Procedures, etc.
Surgical options are not without risks though. While they reduce sleep apnea, in some cases, they can increase cardiovascular symptoms, and quality of life.
Bottom Line
Life cannot be fun when you are in pain. If you are experiencing any issues with your jaw and you feel those painful symptoms associated with sleep apnea in the morning, you should see your dentist immediately.






